Strategizing from 7 cities across the globe
Stress and Sleep Deprivation: A Closer Look at Their Interconnected Role in Hindering Cognitive Functions and Biological Mechanisms
Layla H. Tawbeh


Introduction:
Stress is a common phenomenon that many people face in response to different triggers. Specifically, in the context of university life, academic pressure often drives students to face periods of stress. In fact, multiple sources reveal stress percentages for university students to be consistently elevated over the years and range from above 70% to as high as 88.4% (Asif et al., 2020; Barbayannis et al., 2022; Olson et al., 2025). Though this type of stress can be a mere temporary response of the body, it can still influence routines such as sleep schedules and cycles. The nature of the relationship between stress and sleep is quite complex, and the line between chronic and acute stress alongside lack of sleep and sleep deprivation is important to understanding the complexity of this relationship, as well as the severity of its implications.
What is alerting in this scenario lies within understanding the complexity of sleep cycles themselves. The biologically corresponding function that is linked to each section of sleep cycles can influence cognitive functions such as memory and attention. Likewise, stress also seems to put the effectiveness of said functions at risk. Interestingly enough, the potential correlation between stress and sleep deprivation can possibly affect these cognitive functions in multiple ways. Understanding the directionality of this relationship can bolster our ability at understanding the true extent to which stress – acute or chronic – coupled with lack of sleep, or sleep deprivation, can truly influence our cognitive abilities.
The compelling aspect of the effect on cognitive function lies within how such aspects can influence these functions. This phenomenon is often explained through biological explanations that lie within the range of a neurological basis. However, this basis on its own offers a diverse range of explanations to the hindering of our cognitive functions. Additionally, it is crucial to note the presence of a range of flexibility within these functions, implying incomplete impairment of cognition. Furthermore, different explanations offer an alternate view on the effect on cognitive abilities through impairment of gut microbiota. These multiple insights offer a rather different depth to the range of influence that sleep deprivation and stress put forward.
This research aims to establish the line between what we consider regular sleeplessness and what we consider to be a medical concern, ultimately developing a proper understanding on when lack of sleep becomes sleep deprivation. Moreover, the research attempts to integrate a closer look on the state of academic stress. Establishing this paves the path towards understanding the correlational nature of this interconnected relationship and whether or not it is bidirectional. By doing so, the influence of both stress and sleep deprivation on cognitive functions becomes more evident. What this research uniquely provides is insight into university student demographics in Lebanon through a qualitative survey that will provide real-world applications to this paper, offering a better view on how urgent the situation is for our generation.
Sleep Deprivation:
Generally speaking, sleep deprivation describes the case where a person does not get enough sleep. How much is “enough” sleep depends on the age group an individual falls within. For the target group in this article (18 and above), it is estimated that one should get between 7-9 hours of sleep (Cleveland Clinic, 2022). The key detail for sleep deprivation that we should take into consideration is that it does not necessarily equate to no sleep. In fact, sleep deprivation can occur when a person does not sleep for an adequate number of hours and can also occur when someone’s not attaining quality sleep (Cleveland Clinic, 2022).
Quality of sleep is linked to the sleep cycle mentioned above. Our sleep cycle is divided into a stage of rapid eye movement (REM) sleep and four stages of non-rapid eye movement (NREM) sleep (Cleveland Clinic, 2022). Each of these parts of the cycle with their stages contribute to a different part of bodily functions and entail different physiological changes. This is why the quality and continuity of sleep matter. However, more recently, the American Academy of Sleep Medicine developed only three stages of NREM sleep that are lighter sleep (Stages N1 and N2) and deeper sleep (or SWS; Stage N3) (Iber et al., 2007, as cited in Medic et al., 2017). The key difference between these two classifications lies in the measurement of wake after sleep onset (WASO) and the distribution of NREM sleep stages (Moser et al., 2009, as cited in Medic et al., 2017).
WASO is a key aspect to consider as it affects sleep quality. Wake after sleep is simply what it is said to be; it is the waking period spent in initial sleep. Therefore, a disruption in that would disrupt the quality of sleep. To come to the final findings of this discussion that is posited by Medic et al. (2017), it reveals that long term effects of sleep deprivation in healthy individuals include hypertension, dyslipidemia, CVD, weight-related issues, metabolic syndrome, T2DM, worsening of gastrointestinal disorders, and even increased risks of some cancers and death.
Chronic vs Acute Sleep Deprivation and Their influence on Cognitive Function:
A notable distinction should be made regarding the nature of sleep deprivation. Though it is true that sleep deprivation is a result of not having enough sleep or not getting quality sleep, acute sleep deprivation brings upon variable consequences as compared to chronic sleep deprivation. People experience periods of sleep deprivation, but do typically recover as the cause would be exterior factors such as stress, which will be further discussed, change in routines, or other factors. Sleep deprivation becomes chronic when it is in a consistent state of existence.
Van Dongen et al. (2002) explored the concept of correlation in number of hours of sleep deprivation and cognitive function, where they experimented in test groups with 4, 6, and 8 hours of time in bed per night for 14 consecutive days, as well as a total sleep deprivation experiment involving 3 nights without sleep. Findings revealed that the group with no sleep exhibited markedly larger waking neurobehavioral and sleep delta power responses relative to the amount of sleep lost, compared to the group with only a few hours of sleep. The study notes that there is a nearly linear relation between the lapses in behavioural alertness and the cumulative duration of wakefulness in excess of 15.84 h. The interesting conclusion made from this statement is that the brain functions optimally for 16 hours; hence every hour past that time would induce a linear increase in risk of cognitive lapses regardless of whether the sleep deprivation was for 4 hours, 6 hours, or even no sleep at all.
In a more recent study conducted by Philip et al. (2012), the study group that faced acute sleep deprivation exhibited a higher number of lapses in their reaction time than in the baseline control night with a normal sleep time. The case was similar with chronic sleep deprivation with lapses increasing after the second night. Interestingly though, there wasn't a notable difference in the lapses between chronic and acute sleep deprivation. These findings do resonate with the idea that it is the lack of sleep itself that plays a role in the impediment of cognitive function rather than the number of hours of sleep itself. Another interesting finding in this study indicates that after a recovery night, lapses returned to the baseline number of lapses. Such findings put forward a rather different view on what we typically view the consequences of sleep deprivation to be, raising questions not only on how easy it is to lose some aspects of our cognitive functions, but also how easy it is to restore them back.
Another interesting view is put forward in a very recent study by Choshen-Hillel et al. (2020), where the effects of adding acute sleep deprivation after an hour shift stacked up on accumulated chronic sleep deprivation from hospital shifts are revealed. The two test groups were the residents and the attending physicians who acted as the control groups. The findings in this case were quite diverse, exhibiting a change in some cognitive functions but none in others. For instance, residents exhibited slower processing speed, whereas attention did not differ. Interestingly enough, there was a statistically significant difference between functions in the attending groups relative to the residents. However, the standard deviation bars overlap in chronic and acute residents, implying a statistically insignificant difference. This reveals that adding acute sleep deprivation onto chronic sleep deprivation might not really change cognitive behaviour significantly.
Download the full document
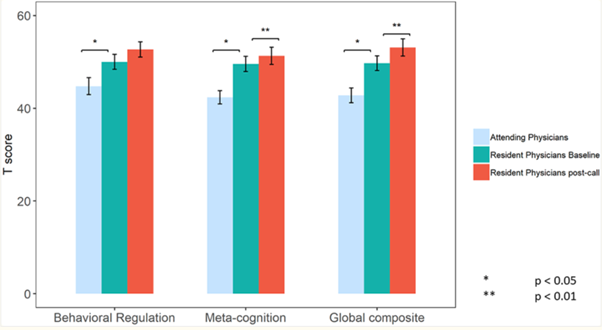
Figure 1: BRIEF-A scores in Attending Physicians and in Resident Physicians both before and after a nightshift (Choshen-Hillel et al., 2020)
Hence, it can be concluded that there is a clear difference between a person that has sleep deprivation and one that doesn't. Yet again, the line between the consequences of acute and chronic sleep deprivation is blurred into approximately non-existence.
Relationship Between Stress and Sleep deprivation:
Stress can be defined as the reaction of a body to changes that occur around a person (Cleveland Clinic, 2024). Stress can arise from multiple different factors which are known as stressors, and this paper specifically focuses on academic stress in the context of University students across Lebanon. It is crucial to understand the relationship between stress and sleep deprivation. It is often that stress co-occurs with sleep deprivation, and the study conducted by Minkel et al. (2012) tests whether this relationship exists due to a simple interaction between sleep deprived individuals and stressors, or whether the relationship is more complex. The findings of the study put forward rather intriguing ideas. While sleep deprived individuals exhibited a greater subjective response to low-stressor conditions compared to those who weren’t, there was no difference between the groups’ responses under higher stressor conditions (Minkel et al., 2012). Hence, we can conclude that the likely mechanism of the relationship between stress and sleep deprivation entails a sort of threshold being lowered to an extent where low stressor conditions can induce an emotional response faster. However, when an event is considered to be a high stressor, then it already triggers the maximum stress response in all participants. Once again, a rather interesting idea is posited where some sort of limit exists in the relationship at hand.
Now, it is crucial to look at how stress affects sleep to understand the bidirectionality of this relationship. In a recent study conducted by Zhang et al. (2024), stress was found to have both a direct and indirect impact on sleep quality. The study puts forward an interesting point: decreased sleep quality itself can be considered a stressor. In turn, a feedback loop is created where sleep quality affects and is affected by stress (Zhang et al., 2024). One explanation to this suggested mechanism lies in how stress can change levels of hormones, such as increasing levels of cortisol and adrenaline, which in turn affect sleep. The compelling aspect of this study is the consideration of how coping mechanisms such as overthinking, emotion-focused coping strategies, and smartphone dependence in response to stress can themselves cause sleep deprivation and lower sleep quality indirectly. Thus, this study provides another aspect and supports the idea that the relationship between stress and sleep deprivation is indeed bidirectional.
Cognitive function and the Sleep Stages:
A valuable aspect in this paper is the consideration of the variable mechanisms at which sleep deprivation is able to affect our cognitive functions. In a study conducted by Khan and Al-Jahdali (2023), we can see the effect of sleep deprivation at different sleep stages. Indeed, there was a different effect on cognitive function that varied depending on the part of the sleep cycle that was disrupted. This aligns with the preceding discussion on the importance of quality sleep in the section of sleep deprivation. To be specific, sleep deprivation in the REM stage has an effect on exciting neurons, which are crucial for assessing danger and in turn relaying a suitable response to stimuli. Sleep deprivation in the NREM stage reduces the release of specific neurotransmitters which would affect sensitivity to such neurotransmitters (Khan & Al-Jahdali, 2023).
Memory and Sleep Deprivation:
Hippocampus activity:
The effect on memory is one cognitive function that is looked at closely in this study. The way memory is disrupted is through the disruption of memory consolidation in the hippocampus through long-term potentiation (Khan & Al-Jahdali, 2023). What was found is that sleep deprivation can alter the surface and shape of glutamate receptors which reduces Ca2+ influx. The importance of this lies in the finding that NDMA receptors, which are responsible for memory consolidation, allow the expression of long-term potentiation through an increased Ca2+ influx (Gais et al., 2008, as cited in Khan & Al-Jahdali, 2023).
Protein Kinase Activity (PKA):
Another aspect regarding memory is in its strengthening. PKA and Cyclic adenosine monophosphate (cAMP) signalling both play a crucial role in doing so. What happens during sleep deprivation is the increase of Phosphodiesterase 4A (PDE4A) enzyme, which is responsible for the degradation of cAMP, and consequently a decrease in PKA activity. This biological explanation is put to the test in a study with mice. It was revealed that in mice that were sleep deprived, PDE4-specific cAMP breakdown increased (Florian et al., 2011, as cited in Khan & Al-Jahdali, 2023).
Cognitive flexibility:
According to Sun et al. (2025), participants with longer sleep deprivation periods exhibited higher inhibitory costs, task-switching costs, switch error rates, and prolonged reaction times across different studies ranging from 2017-2024. However, through the exploration of different studies, Sun et al. (2025) also noted that six other studies showed that cognitive flexibility itself was not impaired, but rather, cognitive processes themselves such as memory, alertness, and attention were. What is even more interesting is that the findings of two studies revealed an improvement in cognitive flexibility. What this raises is that we really still do not know enough about sleep deprivation and cognitive function.
An intriguing aspect to consider again is the mechanism at which sleep deprivation is able to affect cognitive function. The different studies that Sun et al. (2025) discusses involve different explanations and believed mechanisms. For instance, Chan et al. explained that sleep deprivation reduces cerebrovascular activity of specific regions in the brain like the temporo-occipital fusiform cortex and the occipital lobe, and also decreases oxygen supply to some regions. As a result, cognitive flexibility is decreased. This is another mechanism that adds onto the other mechanisms under the section memory and sleep deprivation.
On the other hand, Grant et al. (2017) discusses how sleep deprivation can affect the expression of Brain-Derived Neurotrophic Factor (BDNF) which as a result affects cortical function. This protein acts at the level of the prefrontal cortex (PFC) and hippocampus. Hence, this is why during sleep deprivation, there is reduced activation of the PFC and hippocampus. This is a key detail because both the PFC and hippocampus play a central role in a range of cognitive functions.
Sen et al. (2023) looks at acute sleep depression closely and explains that such short-term acute sleep deprivation can put the body in a state of stress. This specifically targets the secretion of both hormones and neurotransmitters such as cortisol and dopamine respectively. For instance, the secretion of the neurotransmitter dopamine is affected, which is crucial because dopamine plays a role in optimal set-shifting tasks which again brings us back to cognitive flexibility (Girotti et al., 2024). Cortisol, a hormone, is also affected by sleep deprivation.
Gut-brain axis:
There is bidirectional signalling present between the central nervous system (CNS) and the GI tract, which involves signalling between gut microbiota and the brain. Mice were used to experimentally test the effect of sleep deprivation on this gut microbiota (Sun et al., 2023). Two test groups of mice were used in which one group was SPF mice and the other was GF mice. SPF mice simply have a regular gut microbiota, whereas GF mice lack a gut microbiota. Indeed, after the mice were sleep deprived, the recognition index that measured memory was decreased by 24.26% in SPF mice, but no changes were observed in GF mice. To emphasize the findings, GF mice received a transplant of gut microbiota from the faecal samples of humans who had been sleep deprived for 40 hours. These mice were found to exhibit neuroinflammation phenotypes, showing a rather interesting mechanism of how sleep deprivation not only influences cognitive function through the disruption of mechanisms in the brain feedback system, but also negatively interacts with gut microbiota.
Methodology:
The secondary research put forward in the preceding sections explores different aspects including different types of sleep deprivation, its relationship with stress, and the mechanisms at which it affects cognitive function. The primary research conducted involves a qualitative survey with 120 respondents from universities across Lebanon. The survey has four sections: sleep, stress, perceived stress scale, and performance. The aim of this survey is to understand the demographic of Lebanese university students in the context of this paper, and to be able to understand the gravity of the situation.
Data:
According to the survey, 42.5% of respondents sleep for less than 7 hours at least once a week. The statistic involves people who average between 6-8 hours (6 hours of sleep being inadequate). Even when excluding those who receive 7 hours of sleep at least once throughout the week, 34.2 % of respondents reported less than 7 hours of sleep daily. The numbers go as low as a 3-hour average of sleep daily. 15.8% of respondents reported that they have chronic sleep deprivation.
To account for periods of stress, the respondents were asked if their sleep schedule changes during exam season. 87.5% of respondents noted a change in their sleep schedule during exam season. Changes in sleep time go as low as having no sleep at all prior to an exam. The stress demographic itself looks as follows: 80.8% of respondents report a feeling of academic stress and 22.5% of respondents already have some sort of chronic stress. 73.7% of those who have chronic sleep deprivation report having some sort of chronic stress as well.
The survey included a section for a self-assessment known as the perceived stress scale (Cohen et al., 1983). The questionnaire is made up of ten questions which respondents answer through a scale from 0-4, with 0 being never and 4 being very often. The total score is calculated by simply adding the score for each question, minding that questions 4,5,7,8 have a reverse score (0=4:4=0). The higher the score, the higher the perceived stress, and the interpretation of the scores is as follows: 0-13= low stress, 14-26= moderate stress, 27-40= high perceived stress. The results of the survey show that 22.5% of respondents report high perceived stress, 70% report moderate perceived stress, and 7.5% report low perceived stress.
Finally, when asked if respondents have ever noticed a drop in their GPA/grades due to stress/ little sleep, 35% of respondents answered with yes. From those who noted a drop in grades, the drops were as high as 10 grade points and a GPA drop of 0.4 points.
Discussion:
From the findings of this survey, it is clear that university students across Lebanon suffer deeply from sleep deprivation and stress. What makes the findings more concerning is not only the presence of a considerable number of cases of chronic stress and sleep deprivation, but also their co-occurrence that resonates with the secondary research conducted. Additionally, it is evident that sleep deprivation is a common occurrence between university students without even being exposed to academic stress, let alone when students are exposed to it. Overall, the demographic represents a noteworthy amount of sleep deprivation found in the population of study.
What these findings put forward is a need to understand how deteriorating these habits can be for students and how, as secondary research has shown, cognitive function and flexibility can also deteriorate over time. The focal point of concern lies in the nature of the demographic. A significant number of students reveal that they face some sort of sleep deprivation and stress though not chronically diagnosed, and as discussed under the section of the relationship between stress and sleep deprivation, coping mechanisms that people have in response to sleep deprivation can worsen the situation.
Though this area of exploration might seem intuitive at first, the findings reveal just how little we know of the complex relationships at hand. The key detail to this complexity is that though we know that sleep deprivation and disruption can impair cognitive functions like attention, executive performance, and risk-taking behaviours, we do not fully understand the biological mechanisms as to how this works and how reversible it is ( Choshen-Hillel, 2020). Hence, this calls for more focused studies on the biological changes in people that are sleep deprived at first with a more targeted budget towards bridging the gap between this theoretical knowledge that is in itself lacking and how we can turn this into clinical practice and solutions.
One key consideration for this field of study is the need for the development and breakthroughs to be made via personalized medicine. The key idea is that the field of study is already so complex, and the nature of the articles tackled show just how specific and targeted the studies are. Some studies target adults and others target those of older age. Similarly, some studies target groups with genetic SNPs and others without such, as in Grant et al. (2017). The fact that different biological mechanisms are used to explain what is going on and the variable results in each of the targeted studies reiterate the need for the development of personalized medicine.
Another more hands-on method is more dependent on drug-production. What is worth considering is the hurdles the body faces when attempting to respond to sleep deprivation. As discussed above, some biological irregularities involve a dysregulated HPA axis due to increased cortisol and degradation of cAMP. Thus, perhaps promoting efforts towards medically approved treatments that involve drug usage even for short term use could help in promoting translational science. In fact, Arnsten (2015) discusses the concept of using the mechanism of stress leading to loss of PFC function in order to create drugs that could counteract that change and strengthen cognition. This involves once again noting the biological underpinnings of calcium-protein kinase C and cAMP-protein kinase A signalling.
Conclusion:
From the secondary research conducted, it becomes clear that it is not difficult to fall into the cycle of sleep deprivation. We can also understand how sleep deprivation does not only depend on the number of hours of sleep, but also on the quality of sleep itself: 7 hours of sleep does not indicate “good sleep”. Though there is a distinct line between what we consider to be chronic sleep deprivation and acute sleep deprivation, it is not difficult to cross that line.
It is also apparent that there is no one singular rule as to how much sleep deprivation is required to avoid reaching a point of no return. The studies discussed reveal quite interesting findings that explain how there is some sort of limiting factor that comes into play, offering a perspective we wouldn't usually think of. It is apparent that we do not really need to be on 0 hours of sleep to experience symptoms and consequences of sleep deprivation. It is rather a matter of whether we are up after the number of hours in which our body ideally functions or not.
When we place the findings in the context of academic stress, we can see an even more amplified effect as one triggers the other further. This exploration of the relationship between sleep deprivation and stress proved that indeed, there is a strong level of co-occurrence present between these two aspects.
It is also noteworthy to consider the different biological underpinnings of how sleep deprivation affects cognitive function. As can be seen, whether the effect is explained through hippocampus activity or PKA activity, these underpinnings remain a mystery till now, adding more to the complexity of the relationship between sleep deprivation and cognitive performance. What is even more interesting is the extent to which sleep deprivation interacts with our body, even reaching our gut microbiota. Not only that, but it also interacts specifically to bring about negative change.
The primary research conducted only reinforces the importance of finding tangible real-world solutions as sleep deprivation and stress in the Lebanese population of university students is widespread. The deeply complexing nature of the relationship and the presence of an interdisciplinary nature between psychology, neuroscience, biology, and clinical science calls for focused efforts that bridge the gap between conceptual knowledge and real-life solutions.
References
Arnsten, A. F. T. (2015). Stress weakens prefrontal networks: molecular insults to higher cognition. Nature Neuroscience, 18(10), 1376–1385. https://doi.org/10.1038/nn.4087
Asif, S., Muddassar, A., Shahzad, T. Z., Raouf, M., & Pervaiz, T. (2020). Frequency of depression, anxiety and stress among university students. Pakistan Journal of Medical Sciences, 36(5), 971–976. https://doi.org/10.12669/pjms.36.5.1873
Barbayannis, G., Bandari, M., Zheng, X., Baquerizo, H., Pecor, K. W., & Ming, X. (2022). Academic Stress and Mental Well-Being in College Students: Correlations, affected groups, and COVID-19. Frontiers in Psychology, 13, 2. https://doi.org/10.3389/fpsyg.2022.886344
Choshen‐Hillel, S., Ishqer, A., Mahameed, F., Reiter, J., Gozal, D., Gileles‐Hillel, A., & Berger, I. (2020). Acute and chronic sleep deprivation in residents: Cognition and stress biomarkers. Medical Education, 55(2), 174–184. https://doi.org/10.1111/medu.14296
Cleveland Clinic. (2022, August 11). Sleep Deprivation. https://my.clevelandclinic.org/health/diseases/23970-sleep-deprivation
Cleveland Clinic. (2024, May 15). Stress. https://my.clevelandclinic.org/health/diseases/11874-stress
Cohen, S., Kamarck, T., & Mermelstein, R. (1983). A Global Measure of Perceived Stress. Journal of Health and Social Behavior, 24(4), 385–396. https://doi.org/10.2307/2136404
Girotti, M., Bulin, S. E., & Carreno, F. R. (2024). Effects of chronic stress on cognitive function – From neurobiology to intervention. Neurobiology of Stress, 33. https://doi.org/10.1016/j.ynstr.2024.100670
Khan, M. A., & Al-Jahdali, H. (2023). The consequences of sleep deprivation on cognitive performance. Neurosciences, 28(2), 91–99. https://doi.org/10.17712/nsj.2023.2.20220108
Medic, G., Wille, M., & Hemels, M. (2017). Short- and long-term health consequences of sleep disruption. Nature and Science of Sleep, 9, 151–161. https://doi.org/10.2147/nss.s134864
Minkel, J. D., Banks, S., Htaik, O., Moreta, M. C., Jones, C. W., McGlinchey, E. L., Simpson, N. S., & Dinges, D. F. (2012). Sleep deprivation and stressors: Evidence for elevated negative affect in response to mild stressors when sleep deprived. Emotion, 12(5), 1015–1020. https://doi.org/10.1037/a0026871
Olson, N., Oberhoffer-Fritz, R., Reiner, B., & Schulz, T. (2025). Stress, student burnout and study engagement – a cross-sectional comparison of university students of different academic subjects. BMC Psychology, 13(293), 2. https://doi.org/10.1186/s40359-025-02602-6
Philip, P., Sagaspe, P., Prague, M., Tassi, P., Capelli, A., Bioulac, B., Commenges, D., & Taillard, J. (2012). Acute versus Chronic Partial Sleep Deprivation in Middle-Aged People: Differential Effect on performance and sleepiness. SLEEP, 35(7), 997–1002. https://doi.org/10.5665/sleep.1968
Sun, J., Fang, D., Wang, Z., & Liu, Y. (2023). Sleep deprivation and gut microbiota dysbiosis: current understandings and implications. International Journal of Molecular Sciences, 24(11). https://doi.org/10.3390/ijms24119603
Sun, X., Qu, Z., Zhang, X., Zhang, Y., Zhang, X., Zhao, H., & Zhang, H. (2025). The effects of sleep deprivation on cognitive flexibility: a scoping review of outcomes and biological mechanisms. Frontiers in Neuroscience, 19, 1626309. https://doi.org/10.3389/fnins.2025.1626309
Van Dongen, H. P., Maislin, G., Mullington, J. M., & Dinges, D. F. (2003). The cumulative cost of additional wakefulness: Dose-Response effects on neurobehavioral functions and sleep physiology from chronic sleep restriction and total sleep deprivation. SLEEP, 26(2), 117–126. https://doi.org/10.1093/sleep/26.2.117
Zhang, J., Xiang, S., Li, X., Tang, Y., & Hu, Q. (2024). The impact of stress on sleep quality: a mediation analysis based on longitudinal data. Frontiers in Psychology, 15. https://doi.org/10.3389/fpsyg.2024.1431234
